Story Highlights
- A 2017 survey revealed that over half of the American population takes prescription drugs, with four drugs being the average.
- Polypharmacy (taking multiple drugs) poses numerous risks to patients, one of which includes adverse effects from drug-to-drug interactions.
- Receiving multiple vaccines simultaneously also presents potential risks to patients from unknown vaccine-to-vaccine interactions.
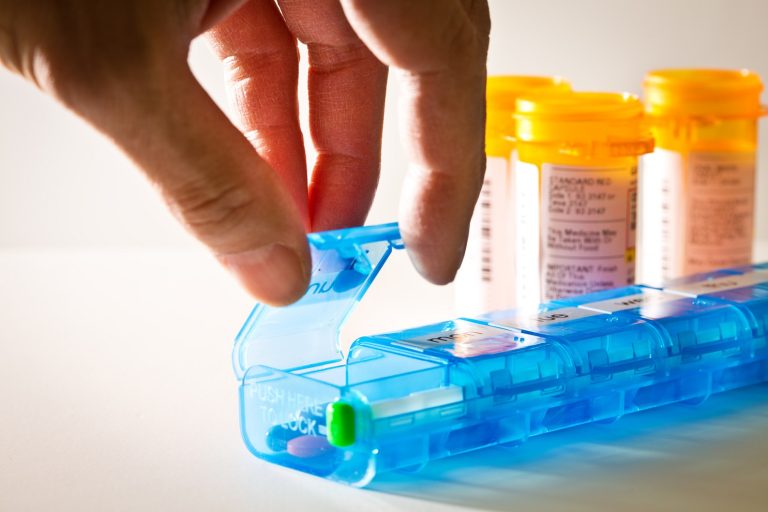
If you are not taking any prescription drugs, you are now the minority. According to a nationally representative Consumer Reports survey conducted in 2017, 55 percent of Americans take a prescription drug, with four drugs per person being the average. The survey found that Americans are taking more pills than ever in our country’s history and no other population in the world consumes as many prescription drugs.1
The total number of prescriptions filled by Americans, for both adults and children, increased by 85 percent over the last 20 years, while the U.S population has increased by only 21 percent.1 In addition, the percentage of Americans taking more than five prescription drugs has tripled over the last two decades.1 The use of multiple medications (both prescription and over the counter drugs) is referred to as polypharmacy.2
In some cases prescription drugs are necessary and appropriate; however, in many cases they are not. In fact, many common health conditions can be counteracted with lifestyle changes (diet, exercises, etc.). Ideally, such changes should be attempted first prior to considering prescription drugs. It is estimated that approximately $200 billion a year is spent on medical care resulting from unnecessary and improper use of medications that doctors routinely prescribe.1
The Dangers of Polypharmacy
Polypharmacy comes with many risks. One of the major risks involves adverse drug interactions.2 Doyle Petrongolo, a pharmacist at Harvard affiliated Massachusetts General Hospital states: “As the number of medications increases, the potential for drug interactions goes up, and there’s an increased potential for side effects that can lead to emergency room visits and hospitalizations.”2
Michael Hochman, MD, at the Keck School of Medicine at the University of South California adds: “The risk of adverse events increases exponentially after someone is on four or more medications.”1
The million-dollar question is why have we reached to this point whereby doctors are prescribing multiple medications to patients? Vinay Prasad, MD, assistant professor of medicine at Oregon Health and Science University provides the following insight:
Many Americans—and their physicians—have come to think that every symptom, every hint of disease requires a drug. The question is, where did people get that idea? They didn’t invent it. They were spoon-fed that notion by the culture that we’re steeped in.1
This cultural shift is attributed a healthcare system that only focuses on symptom management coupled with the intense marketing of drugs and vaccines by the pharmaceutical industry to both physicians and consumers.4
The risks associated with polypharmacy become even greater when patients are under the care of multiple doctors and communication between providers is almost non-existent. According to the Consumer Reports survey, 53 percent of participants taking prescription medication were under the care of two of more doctors.1 Such cases lead to prescribing unnecessary drugs, prescribing repetitive drugs and failing to identify drug interactions.5
But polypharmacy also presents numerous risks under the care of a single doctor. Frequently, polypharmacy makes it challenging to identify the drug that is causing a particular side effect.2 In many cases, doctors’ mistake side effects as symptoms and therefore end up prescribing additional, unnecessary medications that lead to other complications. The result is an endless cycle that fails to address the root cause of the problem.
The rise in “pre-disease diagnoses” has also contributed to polypharmacy. Recent trends in diagnosing patients with “pre-diabetes” or “pre-hypertension,” for example, in cases where medical measurements are slightly elevated but at the higher end of the normal range, has resulted in patients taking drugs prior to the onset of a disease or disorder.1
According to Allen Frances, MD, a professor emeritus at Duke University who studies how the medical establishment expands the definition of diseases and disorders to accommodate expanded prescription drug use: “Lowering the bar for what’s considered normal can also get people on drugs before they need to be. And treating people with drugs at the very early stage of a condition often harms more people than it helps.”1
Vaccine-to-Vaccine Interactions
Similar to the risks associated with drug interactions that stem from polypharmacy, receiving multiple vaccines simultaneously also poses both known and unknown risks to people getting vaccinated; however, the medical establishment often disregards the dangers of vaccine-to-vaccine interactions.
While there are glaring limitations in pre-licensure toxicity testing for individual vaccine ingredients, there is also a lack of basic science research on the synergistic toxicity for all the vaccine ingredients used in the current vaccine schedule recommended by the U.S. Centers for Disease Control and Prevention (CDC).6 In toxicology, synergistic toxicity refers to the effect caused when exposure to two or more chemicals at a time leads to detrimental health effects that are greater than the sum of the individual chemicals.7
According to a report published in BioDrugs:
Many vaccines should not be administered together because of adverse reactions known as vaccine-vaccine interactions, a phenomenon where one vaccine affects another vaccine, thus potentially causing loss of immunogenicity, loss of protective efficacy or induction of adverse reactions. It is important to remember that most vaccine-vaccine interactions are asymptomatic and may only be discovered when the immune status of the vaccine recipient is analyzed or when the individual is challenged by the microbe. The interactions may occur because of physical or chemical interactions within the vaccine formulation, interactions between live vaccines or immunological interference.”8
Similar to prescription drugs, vaccines are also pharmaceutical products that carry potential risks that can be greater for some people than others. Although there are significant gaps in vaccine safety research, individual susceptibility to vaccine reactions for genetic, biological and environmental risk reasons has been acknowledged by the Institute of Medicine.9
Vaccine-to-vaccine interactions are just as dangerous as drug-to-drug interactions and should not be ignored by doctors or by people getting more than one vaccine on the same day.
References:
1 Carr T. Too Many Meds? America’s Love Affair with Prescription Medication.ConsumerReports Aug. 3, 2017.
2 What You Need to Know if You Are Taking Multiple Medications. Harvard Health Publishing June 2016.
3 Parpia R. Medicine’s Symptomatic Focus. The Vaccine Reaction Jan. 22, 2018.
4 Spiegel A. Selling Sickness: How Drug Ads Changed Healthcare. NPR Oct. 13, 2009.
5 Rambhade S. et al. A Survey on Polypharmacy and Use of Inappropriate Medications. Toxicology International 2012; 19(1): 68-73.
6 Parpia R. Big Gaps in Toxicity Testing for Vaccine Safety. The Vaccine Reaction Mar. 26, 2018.
7 Canadian Center for Occupational Health and Safety. Synergism. Government of Canada.
8 Gizurarson S. Clinically Relevant Vaccine-Vaccine Interactions: A Guide for Practitioners. BioDrugs 1998; 9(6): 443-53.
9 Institute of Medicine Committee to Review Adverse Effects of Vaccines. Evaluation of Biologic Mechanisms of Adverse Effects: Increased Susceptibility. (p. 82) Washington, DC The National Academies Press 2012.










4 Responses
Wife was given this flowmax or similar medicine to help with kidney stones. Only took a month and her face swelled up like she fell off a building. Had a long late night emergency room visit and a few hours and then a day after, was better again. Allergic reaction. Doctor quizzed what she was taking, of course, only this one singular medicine. He said; I think I know why you’re having this reaction… Can you imagine trying to figure that out if you’re on 10 different prescriptions? An apple a day keeps the doctor away. Going to hospitals has never been and never will be trendy or cool.
People keep drinking the kool-aid, don’t want to take responsibility for their health, and believe that a magic pill will cure them of everything!
It’s not true people. Wake up. As a population, you are sicker than ever!! Keep lining big pharmaceutical pockets and you will get more and more pills!!
Inner city dependants love going to the hospital, get waited on
Get pills or possibly surgery to brag about. It’s sick behavior
Every other commercial on television is telling people a drug will fix this! Ask your doctor if this drug is right for you! Just like banning commercials for cigarettes, these advertisements should be banned!