- Caused by the bite from an infected tick, Lyme disease is difficult to diagnose, even harder to treat, and the only human vaccine was withdrawn when it was shown to be unsafe.
- Although antibiotic treatment is effective for many people, 10 to 20 percent of Lyme patients suffer from lingering and debilitating symptoms.
- Medical professionals disagree about why some patients fail to heal and suffer chronic symptoms, and some patients turn to alternative therapies to regain their health.
Lyme disease has been around for thousands of years. The tenacious bacteria were found in the 5,300-year-old mummy known as “Ötzi” or the “Iceman,” and Lyme is widely regarded as the most common tick-borne illness in North America.1
Despite pervasiveness of Lyme, currently there is no vaccine approved for use in humans, although one is being developed. An OspA Lyme vaccine manufactured by GlaxoSmithKline was licensed in 1998 by the FDA but was withdrawn by GSK in 2002 amid numerous reports of serious side effects, including vaccine-induced Lyme symptoms and crippling brain and immune system damage. Last year, the FDA approved clinical testing of a new VLA15 Lyme vaccine manufactured by a French biotech firm, Valneva.2
Lyme disease is transmitted via the bite of Ixodes ticks, also known as deer ticks in the east and black-legged ticks on the west coast. In most cases, the disease is transmitted by immature ticks—nymphs as small as poppy seeds—and with a bite so painless many people don’t realize they’ve been bitten at all.3 The disease first gained public attention, and got its name, after a group of children around Lyme, Connecticut, were diagnosed with a mysterious rash and joint pains in the early 1970s.
The strange syndrome was finally linked to a tick bite, and the responsible spirochetes (corkscrew-shaped bacteria) were identified by Willy Burgdorfer as Borrelia burgdorferi in 1981.4
The Great Imitator
One of the problems with diagnosing Lyme disease is that presenting symptoms mimic those of so many other diseases, including chronic fatigue syndrome, fibromyalgia, multiple sclerosis, and psychiatric conditions like depression. Many patients are misdiagnosed and may be inappropriately treated for years before Lyme is diagnosed.
Lyme can affect almost any system of the body, most commonly the heart and joints, and may present as a flu-like illness including fever, chills, sweats, muscle aches and fatigue. Joint and muscle pain are common, and some patients develop a rash or Bell’s palsy, which causes a temporary facial drooping and may be mistaken for stroke.
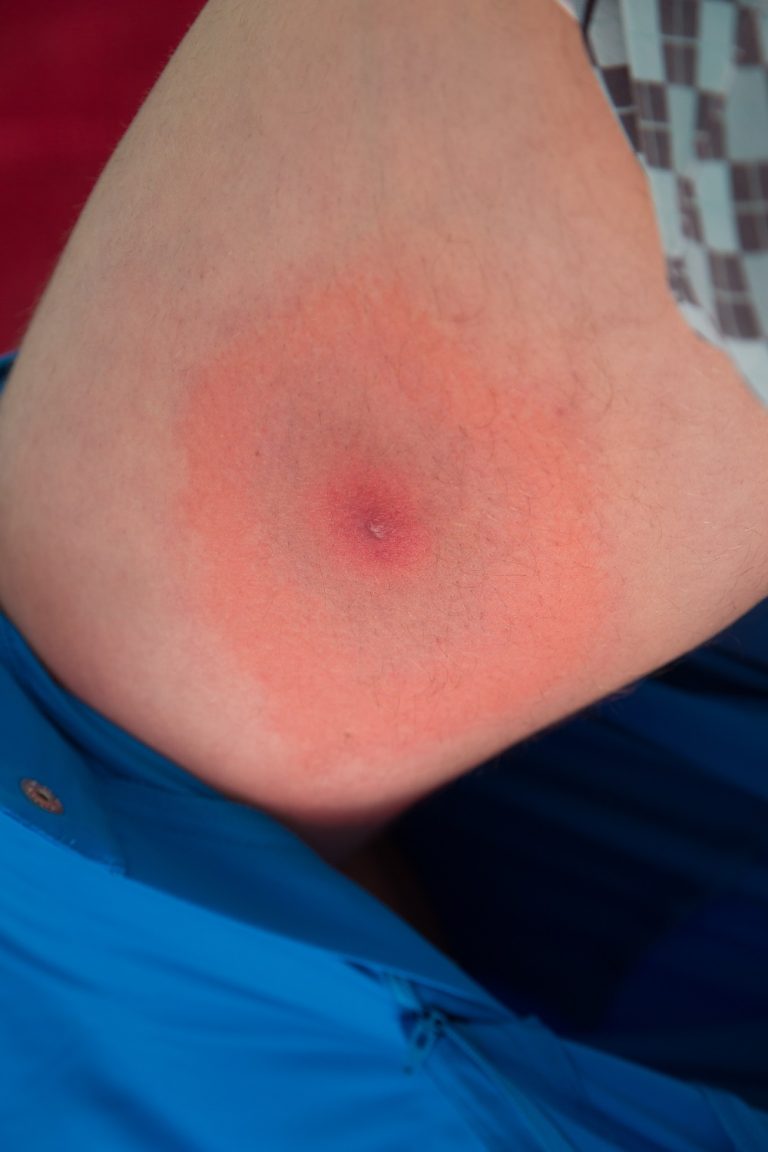
While the classic “bull’s-eye” rash is often seen within a few weeks of being bitten, many people develop a different type of rash, and many never see a rash at all. If a rash does occur, it may resemble a spider bite, a bruise, ringworm, or cellulitis. It may fade over time then reappear, and “satellite” rashes may appear on other parts of the body aside from the site of the tick bite.5
Other common signs of early Lyme include itching, headache, dizziness, stiff neck and swollen lymph glands.6
Blood Testing Is Not Reliable
Currently there are two types of tests for Lyme disease, the enzyme-linked immunosorbent assay (ELISA) and the Western blot. The ELISA is used as a broad screening test, and the Western blot is used to confirm suspicions. Frustrating the diagnosis, neither is a direct test for the infective agent itself. Instead, each test measures the patient’s immune system response to infection: The ELISA checks for the presence of two different antibodies that commonly are present in people with Lyme disease, though they may not show up in the early stages of disease.
The Western blot looks at the pattern of proteins (antigens) in the blood. If five of the ten signature bands are positive, a diagnosis of Lyme is made. However, some of the bands are more significant than others, so that is not a hard and fast rule. Seven of those proteins are common in people with past infection and three tend to indicate the presence of active Lyme.
Unfortunately, blood tests for Lyme are notoriously insensitive, with as many as 20 to 30 percent of tests producing a false-negative result.7 Even more frustrating, a blood sample may come back positive for all ten antigens, “proving” that the patient both has active disease and has been previously infected. Yet, that same patient could undergo treatment, come back the following year with the same symptoms, but their repeat blood test may come back negative for all indications of Lyme.
There are direct tests that also may prove useful, but they tend to be hit or miss because the actual Lyme spirochetes are scarce in blood and so are easily missed on sampling. Culturing of fluid samples in order to grow the Lyme spirochetes holds a lot of promise, but the only available test is new and needs further testing for authentication.
Treatment Isn’t Necessarily a Cure
Unfortunately for sufferers, the standard available treatment for Lyme comprises a thirty-day course of treatment with doxycycline, a broad-spectrum antibiotic that effectively wipes out all bacteria in the body, both the good and the bad. Doxycycline also is associated with numerous side effects, such as gastrointestinal pain and photosensitivity that can make it a difficult course of therapy for many patients.8
Finally, completion of standard treatment is no guarantee of a return to pre-Lyme state of health. Many Lyme sufferers are left with chronic debilitating conditions that compromise their quality of life.
Chronic Lyme: Is it a Thing?
There is a lot of disagreement in the medical community about Lyme and how to diagnose and treat it. The very existence of chronic Lyme disease is debated by medical authorities, though patients who suffer from the debilitating effects of acute Lyme infection have no doubt that chronic Lyme infection is a real and chronic illness. The argument in the medical community seems to hinge not on whether some patients suffer lingering symptoms but on why they experience them.9
The majority of doctors using the standard treatment protocol maintain that the Lyme pathogen is cleared from the body with, at most, a 30-day course of oral antibiotics if caught early. Further, they hold that, even if significant time has passed between the tick bite and diagnosis, a month of intravenous antibiotic therapy will still cure the disease. They do not deny that between 10 and 20 percent of patients develop lingering symptoms, but they refer to that syndrome as “post-treatment Lyme disease” rather than “chronic Lyme disease,” and attribute the symptoms to residual damage to both the tissues and the immune system.
More than simple semantics, those doctors worry that when patients with lasting symptoms are considered to have chronic Lyme infection, the continual treatment they may receive could prevent other health conditions from being appropriately diagnosed and treated. Another concern is the dangers associated with the long-term use of antibiotics and other therapies used to treat chronic Lyme disease.10
Lyme-Literate Doctors Disagree
Physicians identified as “Lyme-literate” have another opinion: They believe that the Lyme bacterium does not always clear from the body but settles in where it can be very difficult to locate, evades the natural immune response, and causes long-term illness.11 These doctors believe that aggressive and long-term treatment with antibiotics, coupled with systemic support measures including herbal treatments may help chronic sufferers to regain their health.
Many natural health practitioners also recommend immune-supportive natural antimicrobials and practices to combat chronic Lyme infection.12
Two Sides Clash Over Therapy for Chronic Lyme Symptoms
Regardless of what it is called, for patients it is the therapeutic predicament that can be most confusing and frustrating. Mainstream medicine asserts that chronic symptoms will ease with enough time, while Lyme-literate practitioners argue that continuing therapy is necessary to combat the sneaky Lyme bacteria.
A cautionary statement by the Centers for Disease Control and Prevention (CDC)13 refers to a study that evaluated various so-called “unorthodox” treatments offered to patients to combat Lyme disease. The researchers looked at more than 30 strategies including oxygen therapies, energy or radiation-based treatment, nutritional approaches, chelation and heavy metal therapies, and unapproved biological and drug therapies. They concluded that there was no scientific support for these therapies and in many cases they could be dangerous.14
Alternatively, even a cursory Internet search turns up myriad testimonials from patients crediting alternative therapies for returning them to health after long battles with chronic Lyme that failed to respond to standard treatment.
References:
1 Kacaijk P, Luytjes W. Vaccination against Lyme disease: Are we ready for it? Human Vaccine Immunotherapy March 2016.
2 La Vigne P, Fisher BL. FDA Gives Green Light to Test Lyme Disease Vaccine on Humans. The Vaccine Reaction Jan. 26, 2017.
3 About Lyme Disease. LymeDisease.org 2017.
4 History of Lyme Disease. Bay Area Lyme Foundation.
5 Early Lyme Disease. LymeDisease.org 2017.
6 Giorgi A. Chronic (Persistent) Lyme Disease. HealthLine Sept. 28, 2012.
7 Lyme Disease Diagnosis. Lyme Disease.org 2017.
8 Doryx Side Effects. Drugs.com.
9 Centers for Disease Control and Prevention. Post-Treatment Lyme Disease Syndrome. CDC.gov. June 26, 2017.
10 MacMillan A. “Chronic Lyme Disease” Isn’t a Real Diagnosis. So Why Are Doctors Prescribing Risky Treatment for It? Health June 23, 2017.
11 Stricker RB. Counterpoint: Long-Term Antibiotic Therapy Improves Persistent Symptoms Associated with Lyme Disease. Clinical Infectious Diseases July 15, 2007.
12 Mercola J. Lyme Disease Treatment Strategies. Mercola.com 2017.
13 CDC. Alternative Treatments for Lyme Disease. CDC.gov. June 15, 2017.
14 Lantos PM et al. Unorthodox Alternative Therapies Marketed to Treat Lyme Disease. Clinical Infectious Diseases Apr. 6, 2015.












19 Responses
I had Lyme disease for at least three years, and maybe longer, before it was diagnosed. I had the ELISA test three times during that period, and it came up negative each time, which is why it took so long for the disease to be correctly diagnosed. It was diagnosed and subsequently treated by a Lyme-literate doctor. It took many months of antibiotics (several different kinds, including doxycycline initially), supplements, and lots of probiotics to counteract the antibiotic effect on my gut flora. I was treated until a month after my symptoms disappeared. So I was effectively cured by a doctor who recognized that chronic Lyme does indeed exist and it can be cured. I am proof, as is a friend of mine in Colorado who had the same experience. The Lyme bacterium is an extremely nasty one, and it has had thousands of years to develop effective countermeasures to the human immune system. It is not to be taken lightly.
Who was your Dr.? My son has suffered his whole life and is almost 22. He had Lyme diagnosis 6-7 yrs ago and only treated w/30 days Doxy. He had another occurance in HS and recently became severely ill again w/Rocky Mtn Spotted Fever. It is another horrible tick born disease but fatal. He is trying to graduate from college in the spring and carry a scholarship but needs a Lyme expert.
Contact http://www.ilads.org/
Well, I don’t know what to say…what a bunch of idiots?
Linda Abernathy, are you a troll or what? Quote – ‘I don’t know what to say? What a bunch of idiots?’ Well.. Perhaps you should be looking in the mirror when you are making such an uninformed and rude remark. Shame on you for your insensitive and callous attitude. We would all be better off if you made no comment at all regarding a subject for which you clearly are not capable of understanding. Please keep your unintelligent thoughts to yourself.
Please don’t counteract rude comments with rudeness. “Do not be overcome by evil, but overcome evil with good”. is a good principle to live by. All people are created in God’s image and are worthy of respect, even if they are deceived or believe differently than you or I do.
Miss Effy, Julie was not rude. She made an appropriate comment to a pointless, rude comment.
Monolaurin from “Inspired Nutrition” offers a comprehensive expose on how the Lyme bacteria tries to hide in the body and reoccurs despite the standard anti-biotic 30 day treatment.
Monolaurin (found in “mother’s breast milk” can actually penetrate the hard exterior shell that the bacteria is protected by.
Please take a look….it has been an enormous success in our family.
Sharon Botto, CNHC
[email protected]
Wondering if anyone has ever heard of Dr Rau from the Paracelsus Clinic in Switzerland. He started treating Lyme’s patients many years ago and what he did was had invited farmers in Switzerland to come be tested for Lyme’s free of charge. What he found out in the test was that 90 % of them tested positive for Lyme’s but they had no symptoms of Lyme’s. Through other testing he treated his Lyme’s patients using natural anti virals and by rebuilding the body. I found that very interesting. I then started reading Medical Medium by Anthony William who also states that Lyme’s is actually a virus and should be treated with natural anti-virals and by rebuilding the body. He stated that these viruses can lay dormant in the body until trauma or injury come into play…then they are released. He has helped many be cured from Lyme’s by this protocol as well. Maybe many need to take another look at this diagnosis as many patients do not get better with a standard protocol of treating for a bacteria.
Many Lyme sufferers have been cured by Rife as in Royal Raymond Rife.
Here you can purchase the best equipment for the job
http://truerife.com/
I have read a lot about this place called Envita. They are located only in Arizona due to the laws there being more friendly towards their type of medical practice. You can youtube them to get more info on why they are located in Arizona and to get testimonies of people who were treated by them. They usually find that infections such as Lyme’s is the underlying cause of other health issues. I would consider going there if I ever should need to.
http://www.envita.com
two words for you…liposomal vitamin c
there has yet to be a bacteria that can withstand appropriate (monstrously large) amounts of vitamin c in the blood stream, which can be done intravenously or with liposomal technology.
vitamin c is expertly effective provided enough is taken (it’s also 100% non toxic in large doses).
do yourself a favor and Google Dr. Fred Klenner
I had lymes several years ago and consulted with a naturopath who gave me a protocol and two things easy to get were sea minerals and colloidal silver. The other came from a compounding pharmacy in OH. I was healthy in 30 days.
got bitten by A tick? swollwn neck ..nerves are shut..creams from drugs did some help But still driving me crazy.medicare would not okay prescriton before PayDay>. so I left finding for myself BATH IN EPSON SALT taken the pain away and drys OUT the bite.
also check out https://weather.com/healidentifying bugs and their bites i live in public housing and for over 6 year we have roaches and bedbugs ..etc etc it is constance fight..they have switch to different pestcontrol companys..but still.
The CDC/IDSA/NIH are what I call the anti-Lyme Cabal. The “science” is done by themselves. They refuse to consider any research outside their paradigm including world wide research and animal studies clearly showing that borrelia persists and changes forms. It also evades the immune system by burrowing into the body as deeply as it can fairly quickly. This is why blood testing doesn’t work. It’s also why standard treatment only works on acute cases. There is also the critical issue of coinfections. If you have Babesia – all the doxy in the world isn’t going to make you better. Each pathogen has its own treatment. Doctors are in the stone ages with this. Yes the immune system is involved and yes it causes autoimmune type symptoms; however, never ever forget that underneath it all is a pathogen invasion that needs to be addressed along with a myriad of other important issues to support the body.
https://madisonarealymesupportgroup.com/2017/07/09/idsa-founder-used-potent-iv-antibiotics-for-chronic-lyme/
https://madisonarealymesupportgroup.com/2017/08/18/drexel-prof-lyme-persists/
https://madisonarealymesupportgroup.com/2016/12/21/dr-zhang-on-persisters/
https://madisonarealymesupportgroup.com/2017/08/25/sleeper-cells-the-stringent-response-and-persistence-in-the-borreliella-burgdorferi-enzootic-cycle/
https://madisonarealymesupportgroup.com/2017/09/02/lyme-disease-and-long-term-antibiotics-contagion-live/
https://madisonarealymesupportgroup.com/2017/08/14/canadian-tick-expert-climate-change-is-not-behind-lyme-disease/
I have late stage disseminated lyme disease. I had this disease for over two decades when I was finally diagnosed in 2011. By that time, I was loosing my vision and hearing, I could no longer think or process what others said to me. I couldn’t remember people or conversations. I could no longer plan or organize, and I couldn’t understand what I read. I often couldn’t walk without support, and there were days where climbing stairs was impossible. My muscles, joints and head ached terribly, and pain relievers and physical therapy couldn’t touch it.
I had to leave my job, of course, and my sister-in-law had to move in to help care for my young children and take care of the house.
The doctors I saw tested for everything, everything except Lyme disease that is. Finally, my son’s pediatrician recommended I visit an LLMD (lyme literate medical doctor) to be tested for Lyme.
I was fortunate: my positive test results along with what I had not realized were obvious lyme symptoms, made the diagnosis clear.
The recovery is not as simple, however.
Six years later, I continue to take antibiotics, many supplements, vitamins and probiotics, I adhere to a very strict diet. I am careful to alternate exertion with plenty of rest.
I am functional now. I can take care of my house, children and myself. While there are still some days when I seem to be back where I started, I have many more good days than bad, which I need to remind myself is a huge improvement.
Slowly, I am getting my life back, but over the years I have met many others whose suffering is just as great or worse. The devastating impact of this disease can’t be overstated. It is understandable that many dismiss Lyme disease, as there is so much misinformation about it. I would only ask, that contrary to our apparent nature to judge and dismiss things we don’t understand, that instead people simply acknowledge their ignorance of the topic, and choose to wish others well with a challenge they themselves have been blessed to avoid.
Thank you to the authors of this article for helping to enlighten readers.
I was diagnosed with Lyme disease in 2005. I was given antibiotics, which seemed to help. However, I still suffer from some of the symptoms, such as chronic fatigue, joint pain, and even neurological problems in controlling hand and leg movements. The inability to walk right etc, are temporary and generally happen when I am really tired and have been working hard. I lost touch with reality.. Suspecting it was the medication I Went off the antibiotics (with the doctor’s knowledge) and started on Lyme disease natural herbal formula I ordered from Natural Herbal Gardens, December 18, 2017 after being on the herbs you recommended, i had a total recovery from Lyme disease with this natural herbal formula treatment. The chronic fatigue, joint pain has subsided. When I stumbled upon you guys, it was just pure instinct. And from that day on it has been one of the best decisions I’ve made in my life. The caring that goes into explaining what herbs work for whatever ails me is astounding. In today’s world where so many are after a quick buck, selling without care, Natural Herbal Garden’s staffs amplifies the difference. I’m a believer in karma, and for generations to come, this is a herbal store that will be leaving it’s footprint in this world. Visit NATURAL HERBAL GARDENS official web site www. naturalherbalgardens. com A world of thanks to The Natural Herbal Gardens!”
I was diagnosed with Lyme disease 5 years ago and was taking Antibiotics and Nonsteroidal anti-Inflammatory drug which seemed to help. However, I still suffer from some of the symptoms. My symptoms have always been chronic fatigue, joint pain, and even neurological problems in controlling hand and leg movements. I am a 54 year old female. the Antibiotics wasn’t really working and I could not tolerate them for long due to severe side effects, so this year our family doctor started me on Natural Herbal Gardens Lyme disease Herbal mixture, We ordered their Lyme disease herbal treatment after reading alot of positive reviews, i am happy to report with the help of Natural Herbal Garden natural herbs I have been able to reverse my symptoms using herbs, my symptoms totally declined over a 8 weeks use of the Natural Herbal Gardens Lyme disease herbal mixture. My Lyme disease is totally reversed! Their official web page is www . naturalherbalgardens . co m this is a herbal store that will be leaving it’s footprint in this world. I’m 54 and have never been this healthier