Many of you reading this probably remember having chickenpox as a child. You were likely tired, feverish and had an itchy rash, which subsequently cleared up, leaving you with lifelong natural immunity. Getting chickenpox was so common it was a rite of passage of sorts, which virtually all school-age children experienced.
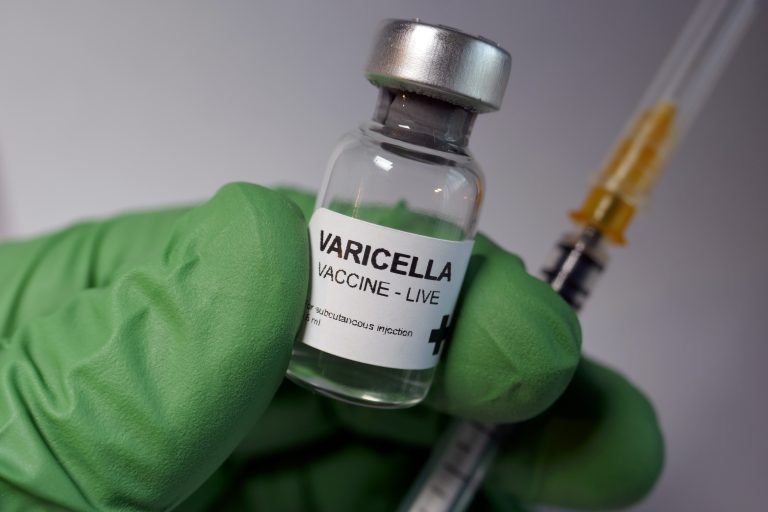
Today chickenpox has become much less common due to the routine administration of the chickenpox (varicella) vaccination. The U.S. Centers for Disease Control and Prevention (CDC) recommends two doses of chickenpox vaccine — the first dose at 12 to 15 months of age and a second dose at age 4 to 6 years.1
They claim it is 90 percent effective at preventing chickenpox (while noting that some people who are vaccinated may still get the disease), which may sound like a success story. But there is much that remains unknown about vaccination and the way it affects human health and disease. Case in point: shingles (herpes zoster).
Shingles is Caused by the Chickenpox Virus
Shingles is caused by the varicella-zoster virus (VZV), the same virus that causes chickenpox. When initially infected, the virus leads to chickenpox, which then lies dormant in your body. Usually, it causes no other problems but in some people the virus reactivates later in life, leading to shingles.
Shingles isn’t typically life-threatening, but it causes a painful rash and sometimes fatigue, headache and fever. In some cases, it leads to postherpetic neuralgia, which is ongoing pain due to nerve damage that can last for months or even years, or neurological problems caused by inflammation of the brain.
While shingles isn’t contagious, an adult who’s never had chickenpox can get the disease after being exposed to someone with shingles. Adults with chickenpox actually experience this disease with more intensified symptoms and have a higher risk of complications, which is why it’s better to have this illness during childhood (and gain the lifelong natural immunity).
Shingles rates are increasing in the U.S., but according to the CDC, “We do not know the reason for this increase.” They then note, “Some experts suggest that exposure to varicella boosts a person’s immunity to VZV and reduces the risk for VZV reactivation. Thus, they are concerned that routine childhood varicella vaccination, recommended in the United States in 1996, could lead to an increase in herpes zoster in adults due to reduced opportunities for being exposed to varicella.”2
In other words, being exposed to chicken pox in the community (or in your household, via your children) may have the protective effect of boosting your immunity against the virus, thereby lowering your risk of shingles as an adult.
Shingles can be prevented by ordinary contact, such as receiving a hug from a grandchild who is getting or recovering from chickenpox. It acts as a natural immunity booster. But with the advent of the chickenpox vaccine, there is less chickenpox around to provide that natural immune boost for children and adults.
The CDC downplays this theory, noting that shingles rates started increasing before the introduction of the chickenpox vaccine and did not accelerate after the chickenpox vaccination program started. However, some research suggests that the chickenpox vaccine may be playing a role in accelerating cases of shingles.
As noted by the National Vaccine Information Center (NVIC), “Today, after chickenpox vaccine has been widely used by children … and has interrupted natural circulation of the varicella zoster virus in the U.S. population, experts believe that half of Americans reaching 85 years of age will experience shingles at some point in their lifetime.”3
Studies Suggest Between Chickenpox Vaccine and Increasing Shingles Rates
In 2016, research published in the American Journal of Epidemiology used mathematical modeling to look into the epidemiology of shingles after chickenpox vaccination. Researchers explained:4
“Given the sparse empirical evidence, mathematical models designed to evaluate the impact of varicella immunization strategies are forced to rely on theoretical, rather than data driven, assumptions to incorporate exogenous boosting assumptions while balancing parsimony in model structure with biological plausibility.
To date, the available formulations of the exogenous boosting hypothesis can be classified into 3 main groups: Despite these structural differences, modeling studies have consistently confirmed the likelihood of a detrimental effect of varicella vaccination on HZ incidence.”
The study analyzed the impact of chickenpox vaccination on shingles epidemiology, as predicted by three models, which revealed that all of the models predicted that chickenpox vaccination lead to an increase in shingles incidence. “Our results reinforce the idea that a better understanding of HZ pathogenesis is required before further mass varicella immunization programs are set out,” the researchers stated.5
In 2005, research by Gary Goldman, PhD also revealed that the chickenpox vaccine could cause a shingles epidemic by limiting wild-type chickenpox virus. He noted, “It may be difficult to design booster interventions that are cost-effective and meet or exceed the level of protection provided by immunologic boosting that existed naturally in the community in the prelicensure era.”6
In other words, you can’t beat Mother Nature, which already had a system in place to keep shingles at bay. In fact, in 2002, research writing in the journal Vaccine presented data confirming that exposure to chickenpox boosts immunity to shingles.
“We show that exposure to varicella is greater in adults living with children and that this exposure is highly protective against zoster [singles],” they wrote, adding that this had serious implications for mass vaccination against chickenpox: “Mass varicella vaccination is expected to cause a major epidemic of herpes-zoster, affecting more than 50% of those aged 10-44 years at the introduction of vaccination.”7
Chickenpox ‘Outbreaks’ Blamed on Unvaccinated
North Carolina recently had an “outbreak” of chickenpox, which was blamed on a school with a number of families claiming religious exemption from vaccines.8 There were at least 36 students affected, with health officials sensationalizing the event with claims that it could spread to the surrounding community.
Remember, while highly contagious, chickenpox typically produces only a mild disease and recovery leaves a child with long-lasting immunity. It’s hardly a newsworthy “outbreak.” Meanwhile, a review of the U.S. chickenpox vaccination program concluded that the vaccine has:
- Not proven to be cost-effective
- Increased the incidence of shingles
- Failed to provide long-term protection from the disease it targets ― chickenpox ― as vaccine efficacy was found to have declined well below 80 percent by 2002
- Is less effective than the natural immunity that existed in the general population before the vaccine was used on a widespread basis in the U.S.
In fact, in 2002, the New England Journal of Medicine published a study of an outbreak of chickenpox that occurred at a day care center despite most of the children having been vaccinated.9 The disease first occurred in a child who had received the chickenpox vaccine three years earlier, and who then infected half of his classmates.
The effectiveness of the vaccine was just 44 percent, and those who had been vaccinated three years or more before the outbreak were at greater risk of contracting chickenpox. According to the study:<10
“In this outbreak, vaccination provided poor protection against varicella … A longer interval since vaccination was associated with an increased risk of vaccine failure. Breakthrough infections in vaccinated, healthy persons can be as infectious as varicella in unvaccinated persons.”
It’s also worth noting that the chickenpox vaccine is made from live, attenuated (weakened) varicella virus. When you or your child get a live virus attenuated vaccine, you can shed vaccine-strain live virus in your body fluids, and the vaccine-strain virus could potentially be transmitted to others, in whom it might cause serious complications. One type of shingles vaccine being administered in the U.S. is also a live-virus vaccine.
Shingles Vaccine Touted as the Solution
The pharmaceutical industry has responded to rising rates of shingles that have possibly been triggered by chickenpox vaccination by creating another shot: a shingles vaccine for seniors. There are two types available in the U.S. Zostavax, a live attenuated vaccine manufactured by Merck, has a dismal effectiveness rate of only 51 percent in adults 60 years and older.11
Merck, by the way, is the same pharmaceutical company that manufactures the chickenpox vaccine. Further, according to NVIC, “[E]fficacy studies showed a significant decrease in vaccine effectiveness one-year post-vaccination and by nine years, Zostavax was determined to be no longer effective at preventing shingles.”12
Shingrix, manufactured by GlaxoSmithKline Biologicals, is a newer two-dose shingles vaccine, licensed in 2017. Although it is said to be over 90 percent effective in adults 50 years and older, it’s a genetically engineered vaccine and, according to NVIC, “no test is available to determine immunity to shingles and long-term vaccine effectiveness is unknown.”
Solving a potentially vaccine-caused shingles epidemic with another vaccine may be creating more problems than it solves. For instance, the CDC notes that, rarely, “live shingles vaccine can cause rash or shingles.”13 vaccine-shoulder-injuries.aspx”>Shoulder pain, fainting and severe allergic reactions have also been noted.
Are There Risks to the Chickenpox Vaccine?
All vaccinations come with risks, and the chickenpox vaccine is no exception. “Reported complications from chickenpox vaccine,” according to NVIC, “include shock, seizures, brain inflammation (encephalitis), thrombocytopenia (blood disorder), Guillian Barre syndrome, death and infection with vaccine strain chickenpox or transmission of vaccine strain chickenpox to others.”14
There are two live virus vaccine for chickenpox in the U.S. (both made by Merck). Varivax contains only chickenpox while ProQuad contains chickenox along with measles, mumps and rubella vaccines. NVIC reported, “A CDC vaccine safety study found that children aged 12-23 months were twice as likely to experience febrile seizures with ProQuad compared to administering MMR and Varivax separately.”15
Perhaps the greatest risk of all of the chickenpox vaccine is that it removes the chance for a person to acquire life-long immunity against chickenpox via natural infection and recovery. Ultimately, the temporary immunity offered via chickenpox vaccination may leave those vaccinated at a heightened risk of more serious disease.
This was a major reason why NVIC did not support the addition of chickenpox vaccine to the mandatory childhood vaccination schedule:16
“The vast majority of children recover from chickenpox disease and do not suffer complications. They are left with a qualitatively superior immunity to the disease. The chickenpox vaccine only gives temporary immunity and leaves older children and adults vulnerable to chickenpox later in life when complications can be much more serious.
Mass use of the chickenpox vaccine by children has eliminated the opportunity for natural asymptomatic boosting of immunity in adults and left adults vulnerable to shingles later in life.”
Note: This article was reprinted with the author’s permission. It was originally published on Dr. Mercola’s website at www.mercola.com.
References:1 U.S. CDC, Chickenpox Vaccine
2 U.S. CDC, Shingles
3 NVIC, What is Shingles?
4 American Journal of Epidemiology, Volume 183, Issue 8, 15 April 2016, Pages 765–773
5 Ibid
6 Int J Toxicol. 2005 Jul-Aug;24(4):205-13
7 Vaccine. 2002 Jun 7;20(19-20):2500-7
8 New York Times November 20, 2018
9 N Engl J Med. 2002 Dec 12;347(24):1909-15
10 Ibid
11 NVIC, How Effective is Shingles Vaccine?
12 Ibid
13 U.S. CDC, Live Shingles VIS
14 NVIC, Chickenpox Disease and Vaccine
15 Ibid
16 Footnote 14











10 Responses
I am a healthy 34-year-old female who recently experienced a shingles outbreak. I, 100% believe that it was due to the lack of natural boosting from exposure to the chicken pox virus during a time when I was under more stress than normal and my immune system weakened. Now my question is…how do we protect our children (who have not been vaccinated against chickenpox) from a more severe outbreak of shingles later in life since there is no way for them to contract chicken pox naturally?
My daughter has been struggling with nerve problems from the herpes zoster virus. She had bells palsy which we learned can come from having vaccines. We finally found out that the root cause for her is aluminum, from vaccines she was given as a child. She is now detoxing the aluminum by drinking a liter of Fiji water every day. It contains silica in high levels, which binds to aluminum and flushes it out. Aluminum can easily be taken by special cells to the brain, I learned from Dr. Christopher Exley, world expert on aluminum from the UK. He recently spoke on this in DC. He found high levels of it in autistic children and adults with memory problems. Anyone who has had a vaccine with aluminum should consider this detox method. If you have mercury, a detox that works is two Brazil nuts per day and two Mercola Liposomol vitamin c. The binding agent for mercury is selenium, found in brazil nuts, and then the vitamin C is a detoxing agent.
Is the Chickenpox Vaccine Creating a Shingles Epidemic?
Just her example of Big Pharma creating future business for itself.
Yes. In 1995 when the CDC allowed the pharmaceutical companies to sell their chickenpox vaccine, the shedding created the shingles epidemic. They use a slightly different chickenpox virus in the vaccine. My experience with this, and other experiences, makes me know DO NOT LISTEN TO YOUR DOCTOR. DO NOT VACCINATE YOUR CHILDREN. They take no responsibility. They are dishonest. They only care about making money. Vaccines are about MONEY not about people. Vaccines are the bread and butter of pediatricians.
I had chickenpox as a child. Our older children had chickenpox before 1995. In 1995 I got shingles, though I’d been recently exposed to natural chickenpox. It was so rare then that the physician did not even know what it was at first. The shingles epidemic was CREATED by the pharmaceutical companies. But now they have a shingles vaccine… Children were not dying of chickenpox. Medical people are so dangerous. The neurologist I know refuses to vaccinate his own children; that is not something he would tell his professional peers.
This article completely misquotes the cdc’s information taken bits out of context to buffer the argument. The quote you took is followed by…”However, two studies have shown that this is not the case… “
please stop spreading misinformation
Anna
What are you referring to? Please be specific in voicing your objections so they can be directly addressed. Otherwise you’re just making a hit and run comment which is typical for people who disagree with something but can’t frame a cogent argument.
My question is if you had chicken pox prior to 1995 and you were required by school to be immunized in the 2000’s , could that increase your chances for shingles because the virus has been dorment in your body and it basically got a boost … Reason I ask is my daughter is 26yr old with shingles..
She had chicken pox twice before 1995 , in her highschool years she was required to have new vaccines that were not required when she originally started school.. because the chicken pox virus was not required , her shot record would not reflect the fact she had already had the virus . So I wonder if the chicken pox vaccine increased her chances of shingles..
“While shingles isn’t contagious, an adult who’s never had chickenpox can get the disease after being exposed to someone with shingles. ” ????? I had chickenpox in the 1960s; in the early 1990s our older children had the chickenpox; in 1995, the same year the chickenpox vaccine came out, I got shingles while in my 30s. It was so rare that the doctor didn’t even know what it was; a woman at church said it looked like shingles so I asked, “Could it be shingles.” He said, “Yes! That’s what it is.” I was pregnant, so did not take the prescription strength Tylenol, but did take some Tylenol to take the edge off. The duration of the infection was about 2 weeks. Why do you say “shingles isn’t contagious,” then say it is?
Bell’s Palsy is on the spectrum of syndromes associated with Lyme Disease. No doubt aluminum in vaccines can harm but she may have as the underlying issue Lyme Disease which mimics many other diseases. IMHO I would get her tested for Lyme Disease look at http://www.lymedisease.org for a Lyme Literate Medical Doctor. Lyme Disease from a tick bite lowers people immune system significantly and a weakened immune system would make you more susceptible to the Shingles. I hope by now she is doing better.